What is an EDI 276 – Health Care Claim Status Request? 
The EDI 276 Health Care Claim Status Request is an ANSI ASC X12 transaction set used by healthcare providers, billing services, clearinghouses, and authorized agents to request the processing status of a previously submitted healthcare claim or encounter.
The transaction enables structured, electronic inquiry into whether a claim has been received, is pending, has been adjudicated, or requires correction, without replacing the original claim submission transaction.
Does the EDI 276 operate within Healthcare and Workers’ Compensation Environments
Yes, the healthcare claim status inquiry operates within defined regulatory and payer ecosystems, thereby aligning EDI 276/277 transaction pair in the following areas:
ASC X12 Standards Governance
The EDI 276/277 transaction pair, structure, hierarchical loops, and segment definitions follow ANSI ASC X12 implementation guides for the Health Care Claim Status Request and for the purpose of discussion several versions were examined, v3051, V4010 and v5010 X12
HIPAA Administrative
The EDI 276/277 transaction pair is mandated under HIPAA for electronic claim status inquiry and response within covered entities.
CMS & Medicare
Medicare Administrative Contractors (MACs) enforce specific companion guides governing allowable identifiers, claim matching rules, and frequency thresholds for 276 submissions.
Workers’ Compensation
State-level workers’ compensation programs—including environments in specific states which define:
- Required hierarchical loops

- Employer-level identification
- Injured worker identification (HL03 = 64)
- Claim administrator reference qualifiers
- Production delimiter standards
Workers’ compensation implementations frequently require additional REF qualifiers and employer-specific identification beyond commercial payer workflows.
Operational Control (Clearinghouse Operations)
Operational Controls imposed by insurers place such as limits on inquiry frequency, identifier validation thresholds, duplicate submissions, suppression and batching; roughly translated this means that internal control (e.g., operational control) must exist in automated environments
Revenue cycles and data governance
Revenue cycles can be impacted in a positive way with automation which also requires vigilance, another word for governance (e.g., operational best practice). Best Practices for achieving positive results in revenue cycles all but requires automated inquiries (e.g., 14-day post-submission trigger). Best Practices for achieving a positive result also means unique tracking identification, validation prior to inquiry, inquiry suppression after adjudication, and precise escalation protocols when the 276/277 transaction pair returns a results beyond what was expected (e.g., SLA.)
Is the EDI 276 Used for Medicare and Medicaid?
Yes. The transaction exists specifically to support electronic claim status inquiry across federally regulated healthcare programs and is used for both Medicare and Medicaid, provided the submitting entity is a HIPAA-covered provider or authorized trading partner.
How Is the EDI 276 Used in Workers’ Compensation?
The  EDI 276 Health Care Claim Status Request is used in workers’ compensation environments to electronically inquire about the processing status of a previously submitted medical claim. The transaction enables providers, billing services, and clearinghouses to determine whether a workers’ compensation payer has received, reviewed, approved, denied, or suspended a claim.
EDI 276 Health Care Claim Status Request is used in workers’ compensation environments to electronically inquire about the processing status of a previously submitted medical claim. The transaction enables providers, billing services, and clearinghouses to determine whether a workers’ compensation payer has received, reviewed, approved, denied, or suspended a claim.
Workers’ compensation workflows differ materially from commercial and Medicare claim cycles. The EDI 276 plays a critical governance role because claim adjudication frequently involves employer validation, managed care organization (MCO) review, and jurisdiction-specific regulatory oversight.
How does PartnerLinQ use the EDI 276?
PartnerLinQ uses the EDI 276 to support automated claim status inquiries between healthcare providers and payers, including commercial insurers, Medicare, Medicaid, and workers’ compensation organizations such as the Ohio Bureau of Workers’ Compensation (BWC). The transaction reduces administrative effort by replacing phone calls, emails, and paper inquiries with a standardized, system-to-system request that integrates directly into payer claim management platforms.
What is the Operational Role of the EDI 276 in State Workers’ Compensation Programs?
State  Workers’ Compensation Program claim status inquiry typically follows this structured lifecycle:
Workers’ Compensation Program claim status inquiry typically follows this structured lifecycle:
- Provider submits medical bill (often via 837 or state-specific format)
- Workers’ compensation payer or BWC receives and logs claim
- Provider submits EDI 276 to request status
- Payer returns EDI 277 Claim Status Response
- Provider monitors outcome and initiates corrective action if required
Unlike commercial insurance, State Workers’ Compensation Program claims may require employer validation and injury verification before adjudication begins. The EDI 276 provides structured visibility into that multi-layered review process.
Can an EDI 276 Be Submitted at the Service-Line Level?
Yes, an EDI 276 can be submitted at the service-line level, provided the payer supports service-level inquiry and the required identifiers are supplied. The ASC X12 276 transaction supports both Claim-Level and Service-Line-Level Inquiry.
Claim-Level Vs. Service-Line-Level Inquiry
| Feature | Claim-Level | Service-Level |
|---|---|---|
| Scope | Entire claim | Specific service |
| Uses SVC Segment | No | Yes |
| Identifies CPT/HCPCS | Optional | Required |
| Used for Partial Denials | Limited | Ideal |
| Required Identifiers | Claim control | Claim + service identifiers |
What responses to the EDI 276 are expected or sent?
The EDI 276 is paired with the EDI 277 Health Care Claim Status Response. Upon receipt of a valid request, the payer responds with an EDI 277 containing claim-level or service-line-level status information. A Functional Acknowledgment (EDI 997) may also be exchanged to confirm syntactic receipt.
What Is the Difference Between EDI 276 and EDI 277?
| Feature | EDI 276 | EDI 277 |
|---|---|---|
| Full Name | Health Care Claim Status Request | Health Care Claim Status Response |
| Direction | Provider → Payer | Payer → Provider |
| Purpose | Request claim processing status | Communicate claim processing status |
| Contains Adjudication? | No | May indicate pending, paid, denied |
| Financial Guarantee? | No | No |
| Initiator | Provider / Clearinghouse | Payer |
| HIPAA Mandated? | Yes | Yes |
| Includes ST/BHT/HL Structure? | Yes | Yes |
| Legal Effect | Informational inquiry only | Informational response only |
What Happens After Submitting an EDI 276?
Submitting an EDI 276 Health Care Claim Status Request initiates a structured electronic workflow between the provider (or clearinghouse) and the payer. While the 276 does not adjudicate the claim, it does trigger a status inquiry process that results in an EDI 277 Claim Status Response, response timing varies by payer. Typically clearinghouse pass-through is ‘near real time’, commercial payers in the same day up to about 48 hours typically, Medicare (e.g., MAC 276 Rules) typically responds within 24 hours, and workers’ compensation varies by state and employer validation.
How to Check Claim Status Electronically Using EDI 276?
Electronic claim status monitoring follows a structured lifecycle. The process begins with claim submission and continues through automated inquiry, response interpretation, and resolution management. Each transaction plays a distinct role within the revenue cycle. Operational walkthrough:
- The lifecycle begins with the EDI 837 Health Care Claim transaction.
- The EDI 276 is triggered after a defined monitoring interval
- Typically, 10–14 days after claim submission or beyond expected cycle
- The payer returns the EDI 277 Claim Status Response.
- The EDI 277 provides status codes describing claim position within the adjudication workflow.
- Analyze and act upon returned status indicators
- Monitor and Interpret EDI 277 Status Codes
- STC01-1 = Claim Status Category Code
- STC01-2 = Claim Status Code
Common 277 Status Categories with STC01 Composite Examples
| STC01 Category | STC01 Status Code | Typical Meaning | Operational Action |
|---|---|---|---|
| A0 | 19 | Claim accepted for processing | Monitor |
| A1 | 20 | Claim rejected | Correct and resubmit |
| A2 | 21 | Missing or invalid information | Review documentation |
| A3 | 562 | Additional information required | Submit supporting documents |
| A4 | 29 | Claim pending review | Monitor |
| F0 | 65 | Claim finalized | Await 835 |
| F2 | 88 | Claim denied | Initiate appeal |
| P0 | 23 | Claim not found | Verify identifiers |
| P1 | 35 | Eligibility issue | Validate coverage |
| R0 | 585 | Awaiting information from provider | Submit requested data |
Is the EDI 276 Required Under HIPAA?
Yes,  and with an important distinction. The EDI 276 Health Care Claim Status Request is part of the HIPAA-adopted electronic transaction standards. However, HIPAA does not require providers to submit claim status inquiries electronically. HIPAA requires that when claim status inquiry is conducted electronically, the standardized X12 276 format must be used, understanding the distinction is critical.
and with an important distinction. The EDI 276 Health Care Claim Status Request is part of the HIPAA-adopted electronic transaction standards. However, HIPAA does not require providers to submit claim status inquiries electronically. HIPAA requires that when claim status inquiry is conducted electronically, the standardized X12 276 format must be used, understanding the distinction is critical.
- HIPAA does not require providers to submit claim status inquiries electronically
- If claim status inquiry is electronically submitted, then the submission MUST leverage the X12 276
What does the EDI 276 support?
The EDI 276 supports claim tracking, claim follow-up, error identification, and payment visibility after a claim has been submitted. The transaction can be used at the summary or service-line level and supports iterative inquiries throughout the claim lifecycle.
Does the EDI 276 Guarantee Payment?
The EDI 276 is an informational inquiry and does not guarantee reimbursement or override payer adjudication policy.
What are the Key Features of the EDI 276?
Key features of the EDI 276 include hierarchical claim identification, traceability through reference and control numbers, support for monetary and service detail, and direct pairing with the EDI 277 response. The transaction supports both healthcare and workers’ compensation use cases under HIPAA-compliant exchange models.
features of the EDI 276 include hierarchical claim identification, traceability through reference and control numbers, support for monetary and service detail, and direct pairing with the EDI 277 response. The transaction supports both healthcare and workers’ compensation use cases under HIPAA-compliant exchange models.
What Is the Purpose of the EDI 276 Transaction?
The purpose of the EDI 276 is to provide a reliable, standardized, and auditable mechanism for determining the processing status of a submitted healthcare claim. The transaction removes uncertainty from post-submission workflows by allowing providers to understand whether a claim has been received, is under review, has been finalized, or requires corrective action before resubmission.
How Often Can an EDI 276 Be Submitted?
The frequency of submitting an EDI 276 Health Care Claim Status Request is controlled by payer, defined in EDI companion guides, clearinghouse rules, State Medicaid or State Workers’ Compensation Program policies and internal governance relative to revenue cycle, Understanding the payers, layers, and HIPAA guidance is essential to avoid rejection or transaction throttling. Remember HIPAA standardizes the format of the transaction but does not mandate how often it may be sent
- Frequency is not defined by HIPAA.
- HIPAA does not require providers to submit claim status inquiries electronically
- If claim status inquiry is electronically submitted, then the submission MUST leverage the X12 276 (HIPAA)
What are the Required Data Elements and Identifiers in the EDI 276?
The EDI 276 typically includes identifying information for the provider, payer, injured worker or patient, and claim, along with service dates, monetary amounts, procedure identifiers, and trace numbers required to uniquely identify the claim being referenced.
A valid EDI 276 as a practical matter must contain information sufficient to uniquely match
The EDI 276 transaction does not resubmit the claim, rather it provides an automated matching data response. In short, the inquiry must match the original 837 exactly which means the data included such as claim control numbers, member IDs, date of service, and billed amount must be precise or the query (276) will fail to return a result (277).
Required information generally falls into five categories:
While payer companion guides may differ and define additional situational requirements, generally speaking matching accuracy determines whether the payer can return a meaningful 277 response, thus quality identifiers, those one could reasonably expect to return a quality response, fall into four primary categories with payer companion guides possibly imposing additional situational requirements:
- Transaction Data
- Transaction control identifiers
- Claim control number
- Patient ID
- Hierarchical structure data
- Provider identifiers (NPI)
- Claim-level (and optional service-level) identifiers
- Patient or injured worker identifiers
- Date of service
- Total billed amount (when required)
EDI 276 Structure and Technical Composition
What are the Essential Components of the EDI 276?
The EDI 276 Health Care Claim Status Request is composed of a defined set of hierarchical loops and supporting segments that together provide sufficient context for a payer to identify a previously submitted claim and determine its current processing status. These components ensure that inquiries are precise, traceable, and auditable across healthcare and State Workers’ Compensation Program environments.
Each component plays a distinct role in narrowing the scope of the inquiry, from identifying the requesting and responding parties, to isolating a specific claim or service line, to providing the temporal and financial context required for accurate status reporting.
| Component Category | Description | Business Purpose |
|---|---|---|
| Transaction Control | ST / SE segments | Establish transaction boundaries and control integrity |
| Hierarchical Structure | BHT / HL segments | Define the inquiry context and entity relationships |
| Party Identification | NM1 | Identify the provider, claimant, and payer |
| Traceability | TRN / REF | Correlate the inquiry to a specific claim |
| Financial Context | AMT | Identify the monetary scope of the inquiry |
| Temporal Context | DTP | Specify service, submission, or processing dates |
| Service Detail | SVC | Identify individual services being inquired upon |
What are the Common Segments included in the 276?
The following segments appear consistently across EDI 276 implementations and form the structural and informational foundation of the claim status inquiry. Together, these segments allow payers to reliably interpret the request, locate the referenced claim, and return an appropriate response through the EDI 277.
| Segment | Name | Functional Role |
|---|---|---|
| ST | Transaction Set Header | Begins the transaction and identifies the request |
| BHT | Beginning of Hierarchical Transaction | Indicates inquiry intent and timing |
| HL | Hierarchical Level | Organizes the inquiry by entity and claim |
| NM1 | Individual or Organizational Name | Identifies involved parties |
| TRN | Trace | Uniquely identifies the inquiry |
| REF | Reference Information | Supplies claim and control identifiers |
| AMT | Monetary Amount | Indicates claim or service amount context |
| DTP | Date or Time or Period | Identifies relevant service or processing dates |
| SVC | Service Information | Identifies specific services under inquiry |
| SE | Transaction Set Trailer | Ends the transaction |
Summary Table of Key Segments
| Segment | Primary Use |
|---|---|
| ST | Transaction identification |
| BHT | Inquiry intent |
| HL | Structural hierarchy |
| TRN | Claim correlation |
| SVC | Service-level inquiry |
What Status Codes are used with the EDI 276?
| Status Category | Where Used | Business Purpose |
|---|---|---|
| Purpose Codes | BHT02 | Identifies original status request |
| Hierarchical Codes | HL03 | Identifies entity and inquiry level |
| Service Identifiers | SVC01 | Indicates service under review |
Status indicators in the EDI 276 communicate the type and scope of the claim status being requested, not the adjudicated outcome itself. Status context is conveyed through hierarchical codes, reference qualifiers, and service identifiers that define whether the inquiry is claim-level or service-level.
What Reason Codes are used with the EDI 276?
| Reason Category | Where Used | Business Meaning |
|---|---|---|
| Reference Qualifiers | REF01 | Identifies claim or policy context |
| Date Qualifiers | DTP01 | Explains timing relevance |
| Monetary Qualifiers | AMT01 | Clarifies financial scope |
Reason-oriented indicators within the EDI 276 clarify why a particular claim or service is being referenced. These codes provide context for the inquiry and guide the payer in selecting the appropriate status information to return in the EDI 277 response.
What Use Cases does the EDI 276 support?
The EDI 276 supports a range of post-submission claim management and visibility use cases by providing a standardized method for requesting claim status information after a claim has been filed. These use cases are especially critical in high-volume healthcare and State Workers’ Compensation Program environments where timely insight into claim processing directly impacts cash flow and operational efficiency.
| Use Case | Description | Primary Stakeholders |
|---|---|---|
| Claim Receipt Verification | Confirms that a claim was received and accepted for processing | Providers, Clearinghouses |
| Claim Processing Tracking | Determines whether a claim is pending, in review, or finalized | Providers, Payers |
| Denial and Delay Follow-Up | Identifies reasons for claim delays, rejections, or denials | Billing Services, Providers |
| Workers’ Compensation Claim Monitoring | Tracks the status of injury-related medical claims | Providers, Ohio BWC |
Common EDI 276 Errors and Rejection Scenarios
The EDI 276 does not adjudicate claims, it is an inquiry which means that it must match an existing claim record precisely. When identifiers or structure do not align, the payer cannot return a meaningful status. An EDI 276 Health Care Claim Status Request fails for one of three primary reasons:
- Structural validation failure
- Identifier mismatch
- Operational timing or frequency violation
Understanding these categories allows revenue cycle teams to diagnose rejection quickly and prevent recurring submission errors.
How the EDI 276 work in Workers’ Compensation Environments?
State Workers’ Compensation Program workflows differ from commercial and Medicare (e.g., Medicare MAC 276 Rules) claim cycles because adjudication frequently involves employer validation, managed care organization (MCO) review, and state regulatory oversight.
The EDI 276 from that perspective, provides structured visibility into that multi-layered review process.
Workers’ Compensation Claim Lifecycle
The 276 requests visibility into the current adjudication stage and does not alter claim status. A typical workers’ compensation status workflow follows these stages:
- Provider submits medical bill (often via EDI 837 or state-specific format)
- Claim enters payer or Bureau of Workers’ Compensation (BWC) intake system
- Employer or claims administrator validates injury
- Medical review and adjudication occur
- Provider submits EDI 276 to request status
- Payer returns EDI 277 Claim Status Response
What are the Benefits of the EDI 276?
The EDI 276 delivers measurable operational and financial benefits by replacing manual claim status follow-up processes with a standardized, automated inquiry. These benefits become increasingly significant as claim volumes grow and payer response times vary.
| Benefit | Description | Business Impact |
|---|---|---|
| Automation | Eliminates phone calls, emails, and paper inquiries | Reduced administrative cost |
| Transparency | Improves visibility into claim processing stages | Faster issue resolution |
| Accuracy | Uses standardized identifiers and references | Fewer inquiry errors |
What are the Benefits of Automating Claim Status Monitoring with EDI 276?
Automating claim status monitoring with the EDI 276 reduces AR aging, lowers administrative burden, accelerates denial resolution, and strengthens revenue cycles. The transaction provides structured electronic visibility into claim processing. Automation converts that visibility into measurable operational and financial performance improvement. Automation determines whether that visibility produces operational leverage.
| Benefit Area | Measurable Impact |
|---|---|
| AR Days | Reduction through earlier follow-up |
| Staff Time | Decrease in manual status calls |
| Denial Rate | Faster identification and correction |
| Cash Flow | Improved predictability |
| Compliance | Improved audit documentation |
| Workers’ Comp Processing | Reduced employer-validation delays |
How efficient is the EDI 276?
The EDI 276 replaces repeated phone calls and manual status checks with a single automated inquiry. When fully automated (e.g., paired with the EDI 277) the transaction provides near real-time insight into claim processing, significantly reducing delay and administrative overhead.
How Compliant is the EDI 276?
The  EDI 276 aligns with ANSI ASC X12 standards and supports HIPAA-mandated claim status inquiry workflows. The transaction is designed to operate within regulated healthcare and workers’ compensation environments while maintaining auditability and data security.
EDI 276 aligns with ANSI ASC X12 standards and supports HIPAA-mandated claim status inquiry workflows. The transaction is designed to operate within regulated healthcare and workers’ compensation environments while maintaining auditability and data security.
The EDI 276 transaction is one of the HIPAA-mandated administrative transaction standards for electronic claim status inquiry. Remember HIPAA standardizes the format of the transaction but does not mandate how often it may be sent
- Frequency is not defined by HIPAA.
- HIPAA does not require providers to submit claim status inquiries electronically
- If claim status inquiry is electronically submitted, then the submission MUST leverage the X12 276 (HIPAA)
What is the Format of the EDI 276?
The EDI 276 uses a hierarchical ANSI X12 format and is transmitted within the HR Functional Group. The structures discussed in this document v3051, V4010 and v5010 support both claim-level and service-level inquiries and mirror the response structure used by the EDI 277, also HR Functional Group v3051, V4010 and v5010 X12.
How Accurate is the EDI 276?
Accuracy, as you might expect depends on the use of valid claim identifiers, consistent reference values, and adherence to implementation guidance defined by payers and regulatory agencies. Accuracy is critical to support automated claim status inquiries between healthcare providers and payers. The EDI 276 transaction enables a structured, electronic inquiry into whether a claim has been received, is pending, has been adjudicated, or requires correction, without replacing the original claim submission transaction. The transaction reduces administrative effort by replacing phone calls, emails, and paper inquiries with a standardized, system-to-system request that integrates directly into payer claim management platforms.
What are the Limitations of the EDI 276?
Limitations include dependency on payer processing timeliness and the informational nature of the response, which does not itself authorize payment or guarantee adjudication outcomes.
Are Guidelines and Sample Files available for the EDI 276?
Guidelines and sample files are available through trading partners and operators like PartnerLinQ to support onboarding and technical development.
EDI 276 Example File (X12 Sample – 005010X212)
BHT*0010*13**20030109~
HL*1**20*1~
NM1*PR*2* PAYER NAME *****21*9012345918341~
PER*IC*PROVIDER CONTACT INFO*TE*6145551212~
HL*2*1*21*1~
NM1*41*2******46*111222333~
HL*3*2*19*1~
NM1*1P*2*PROVIDER NAME*****FI*FEDERAL TAX ID~
NM1*1P*2*PROVIDER NAME*****XX*NPI NUMBER~
NM1*1P*2*PROVIDER NAME*****SV*PROVIDER NUMBER~
HL*4*3*22*1~
NM1*IL*1*DOE*JOHN****MI*MEMBERID~
TRN*1*500~
HL*5*4*23~
DMG*D8*19171106*F~
NM1*QC*1*DOE*JANE~
TRN*1*500~
AMT*T3*68.69~
DTP*232*RD8*20021016-20021016~
SE*21*0046~
What are the Basic Questions for EDI Integration with the EDI 276?
The following questions frame the technical, operational, and governance considerations commonly encountered when integrating the EDI 276 Health Care Claim Status Request. These questions reflect patterns observed across PartnerLinQ implementations and mirror the integration depth applied to the EDI 148.
| Integration Question | What to Evaluate | Why It Matters |
|---|---|---|
| Are samples and specifications available? | Availability of X12 and payer-specific guides | Accelerates onboarding and testing |
| What is the general direction of the transaction? | Outbound inquiry from provider or intermediary | Defines system roles and routing |
| Is the transaction inbound or outbound? | Role-based behavior across providers and payers | Drives mapping and monitoring design |
| What response to the transaction is expected or sent? | Requirement for EDI 277 Claim Status Response | Completes the inquiry lifecycle |
| Are response samples and specifications available? | Access to 277 examples and rules | Improves testing and exception/error handling |
| Are there other interested parties? | Clearinghouses, TPAs, MCOs | Expands coordination scope |
| What transactions might these parties participate in? | 837, 277, 997 | Enables end-to-end workflow planning |
| How are changes or follow-ups handled? | Repeat inquiries versus manual escalation | Impacts operational workload |
| Is the transaction triggered automatically or manually? | System events versus user-driven requests | Defines automation opportunities |
| Are responses automatically processed? | Automated interpretation of 277 responses | Improves velocity and visibility |
| Are jurisdiction-specific rules encountered? | State or payer constraints may exist on inquiry content | Prevents misinterpretation and compliance issues |
What Business Level Workflow does the EDI 276 support?
The EDI 276 Health Care Claim Status Request operates within a broader healthcare EDI ecosystem. The 276 does not operate in isolation. It serves as a governance checkpoint between claim submission and payment confirmation. The transaction interacts with claim submission, acknowledgment, response, and remittance workflows, supporting post-submission claim monitoring workflows. Post-submission claim workflows enable providers to track claim progression, identify issues before they impact cash flows, and take corrective action without resubmitting claims.
Operational Relationship Summary
| Transaction Type | Impact on 276 Monitoring |
|---|---|
| Pre-Claim Reporting (148) | Establishes workers’ comp claim foundation |
| Eligibility (270/271) | Prevents downstream 276 dependency |
| Claim Submission (837) | Required prerequisite |
| Documentation (275) | Triggered by 277 requests |
| Status (276/277) | Provides claim visibility |
| Payment (835) | Confirms financial resolution |
| Technical Acks (997/999) | Validate transport and structure |
| Application Errors (824) | Identify business-level issues |
Workers’ Compensation Claim Workflow Example
Optional and Manual transaction options shown to provide context
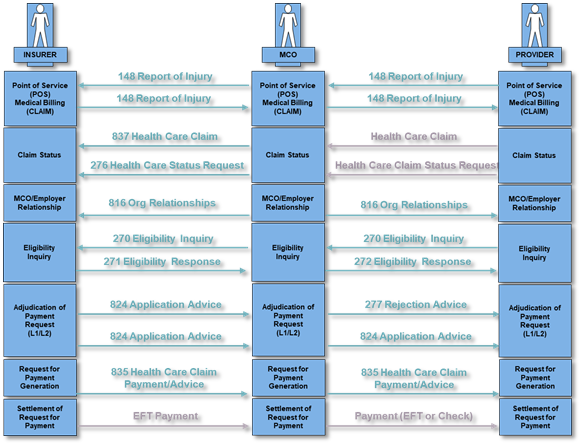
Workers’ Compensation Example Flow 
148 → 837 → 276 → 277 → 275 (if required) → 835
Commercial / Medicare Example Flow
270 → 271 → 837 → 999 → 276 → 277 → 835
What are the Best Practices for using the EDI 276?
The EDI 276 Health Care Claim Status Request acts as a visibility tool, more so than a payment mechanism. Effective use of the EDI 276 requires disciplined timing, precise identifiers, payer-specific alignment, automated cadence, and accurate interpretation of 277 status codes. Where the 276 provides visibility, governance delivers performance.
| Best Practice | Description | Benefit |
|---|---|---|
| Use consistent identifiers | Match claim control numbers | Accurate responses |
| Validate Identifiers Before Submission | Confirm billing provider NPI, member ID, claim control number, date of service, and billed amount match the original 837 exactly. | Improves successful claim matching and lowers rejection rates. |
| Align With Payer Companion Guides | Configure transaction structure, REF qualifiers, loop requirements, and frequency limits according to payer-specific rules. | Prevents structural and business-level rejections. |
| Submit at the Proper Time | Initiate the first 276 inquiry only after a reasonable claim processing window (typically 10–14 days post-837 submission, unless payer guidance specifies otherwise). | Reduces “claim not found” responses and avoids unnecessary rework. |
| Automate Inquiry Cadence | Use aging thresholds and SLA triggers to systematically generate inquiries instead of relying on manual follow-up. | Reduces AR days and standardizes monitoring discipline. |
| Automate follow-ups | Trigger inquiries systematically | Reduced workload |
| Suppress Duplicate Submissions | Implement logic to prevent repeated 276 inquiries within short intervals or after adjudication. | Avoids throttling, trading partner friction, and unnecessary transaction costs. |
| Use Service-Level Inquiry Strategically | Submit service-line-level 276 only when partial adjudication or line-specific discrepancies occur. | Speeds resolution of targeted issues without resubmitting entire claims. |
| Log TRN for Traceability | Capture and store TRN segment values to correlate 276 inquiries with 277 responses. | Strengthens audit trail, reconciliation accuracy, and compliance readiness. |
| Interpret 277 STC Codes Correctly | Parse STC01 composite codes to determine whether claims are pending, denied, finalized, or require documentation. | Enables faster denial resolution and operational action. |
| Integrate 276 Monitoring Into KPIs | Track metrics such as aging by status, denial detection interval, and pending claim duration. | Improves financial forecasting and executive visibility. |
| Monitor responses | Track EDI 277 outcomes | Faster resolution |
| Implement Exception-Based Monitoring | Prioritize high-dollar or aged claims for early inquiry and escalation. | Focuses resources where financial risk is greatest. |
| Coordinate With 275 for Documentation | Submit EDI 275 attachments promptly when a 277 indicates additional information is required. | Accelerates adjudication and reduces prolonged pending status. |
| Tailor Approach for Workers’ Compensation | Include employer loop, date of injury, and state claim number where required; allow for longer employer validation cycles. | Improves match success and reduces premature inquiries in workers’ compensation environments. |
| Stop Inquiry After Finalization | Suppress further 276 submissions once 277 indicates final adjudication or 835 remittance is received. | Eliminates unnecessary transactions and reduces administrative overhead. |
Organizations that operationalize the 276 as a structured monitoring instrument rather than a reactive inquiry, achieve measurable improvements in revenue cycle and financial performance.
Best Practices for Using the EDI 276
Best practices, given the use cases available here, center on timing, precision, automation, governance, and payer alignment.
What Transactions are associated with the EDI 276?
The EDI 276 Health Care Claim Status Request transaction does not function independently, rather it operates within the broader healthcare EDI ecosystem interacting with claim submissions, acknowledgments, response, and remittance workflows.
Summary Table of Associated Transactions
| ID | Name | Category | Purpose | Relationship to 276 |
|---|---|---|---|---|
| 148 | Report of Injury, Illness or Incident | Workers’ Compensation Reporting | Submit first notice of injury (FROI) to state or insurer | May precede claim creation in workers’ compensation; establishes claim context later monitored via 276 |
| 837 | Health Care Claim | Claim Submission | Submit medical claim for adjudication | Creates the claim record that the 276 inquires about |
| 270 | Eligibility, Coverage or Benefit Inquiry | Eligibility Verification | Verify patient coverage before rendering services | Helps prevent claim denial that would later require 276 monitoring |
| 271 | Eligibility, Coverage or Benefit Response | Eligibility Response | Returns coverage and benefit information | Reduces downstream claim status inquiries by validating eligibility upfront |
| 275 | Additional Information to Support a Claim | Claim Attachment | Transmits supporting documentation (e.g., medical records) | Often triggered after a 277 indicates additional information required |
| 276 | Health Care Claim Status Request | Status Inquiry | Request processing status of submitted claim | Central monitoring transaction |
| 277 | Health Care Claim Status Response | Status Response | Communicates claim processing status | Direct response to 276 |
| 816 | Organizational Relationships | Information Maintenance | Trading partner or payer relationship master data | Supports trading partner configuration that enables 276 routing |
| 824 | Application Advice | Application-Level Error Reporting | Reports business-level transaction errors | May report content errors related to 276 submissions |
| 835 | Health Care Claim Payment / Remittance Advice | Payment | Communicates payment, denial, and adjustments | Financial conclusion of lifecycle monitored by 276 |
| 997 | Functional Acknowledgment | Technical Acknowledgments | Confirms receipt of transaction set | Confirms 276 receipt at functional level |
| 999 | Implementation Acknowledgment | Technical Acknowledgment | Validates structural compliance with implementation guide | Confirms 276 format compliance before status processing |
Footnotes
- PartnerLinQ EDI 276 Implementation Guidance.
- ANSI ASC X12, Transaction Set 276 – Health Care Claim Status Request.
- Ohio Bureau of Workers’ Compensation EDI 276 v3051 Specification.
Explore Our Integration Solutions
PartnerLinQ Integration Solutions
Connect Everything. Integrate Intelligently.
Future-Proof Your Business with Composable, AI Powered Connectivity.



