What is the EDI 148 – Report of Injury, Illness or Incident? 
The EDI 148 Report of Injury, Illness or Incident is an ANSI ASC X12 transaction set used to electronically report workplace injuries, illnesses, or incidents. The transaction standardizes the capture and exchange of incident data for statistical reporting, legal compliance, claims initiation, and risk management within workers’ compensation and insurance ecosystems.
How does PartnerLinQ use the EDI 148?
PartnerLinQ uses the EDI 148 to enable employers and healthcare providers to report workplace injuries, illnesses, or incidents into workers’ compensation and insurance systems that administer compensatory benefits. The transaction initiates claim workflows, supports regulatory compliance, and enables downstream eligibility, coverage, and claims processing.
The EDI 148 Report of Injury, Illness or Incident is a standardized ANSI X12 EDI designed to facilitate the exchange of information between employers, insurance carriers, third-party administrators (TPAs), and state agencies.
What responses to the EDI 148 are expected or sent? 
Trading partners typically return an EDI 997 Functional Acknowledgment to confirm syntactic receipt of the EDI 148. Trading partners may use AS2 for communication between them incorporating the MDN (Message Delivery Notifications) as well. Additional business-level responses may occur through downstream transactions, including eligibility inquiries, claims processing workflows even EDI 824 Application Advice, an electronic document used to report the status (acceptance, rejection, or required changes) of a previously sent transaction.
What does the EDI 148 Report of Injury, Illness or Incident support?
The EDI 148 supports first reports of injury, illness, or incident, subsequent updates to previously reported incidents, and ongoing synchronization of claim-related data across employers, insurers, third-party administrators (TPAs), healthcare providers, and regulatory agencies.
What are the Key Features of the EDI 148?
Key features include key data elements, standardized incident reporting, hierarchical data structuring, support for employment and wage context, and compatibility with regulatory and jurisdiction-specific implementation guidelines.
What is the Purpose of the EDI 148 Report of Injury, Illness or Incident?
The purpose of the EDI 148 is to provide a reliable, auditable, and standardized mechanism for reporting workplace incidents that trigger workers’ compensation and insurance claim processes by establishing the data contents for reporting an injury, illness or incident.
What Information is Included in the EDI 148?
The transaction includes employee identification, employer details, incident description, medical context, employment status, wage and schedule information, and insurance or claim administration references.
Key Data Elements in an EDI 148 Report of Injury, Illness or Incident Transaction include:
- Employee Details (name, SSN, date of birth, employment status)
- Employer Details (company name, address, industry classification)
- Incident Details (date, time, location, and description of the injury/illness)
- Medical Information (type of injury, body part affected, initial treatment)
- Witness and Supervisor Information (if applicable)
- Insurance Information (policy number, claim administrator details)
What are the Essential Components of the EDI 148?
| Component Category | Description | Business Purpose |
|---|---|---|
| Transaction Control | ST / SE segments | Establish transaction boundaries and control counts |
| Hierarchical Structure | BHT / HL segments | Define reporting context and parent–child relationships |
| Party Identification | NM1 / N3 / N4 / PER | Identify employers, employees, insurers, and contacts |
| Incident Reporting | CRI / DTP / CRC | Describe injury, illness, or incident conditions |
| Employment Context | ESI / EMT / TPB | Define employment status and job context |
| Financial Context | AMT / AIN / QTY / WS | Support wage, income, and schedule reporting |
| Government Reporting | GRI | Enable statistical and regulatory reporting |
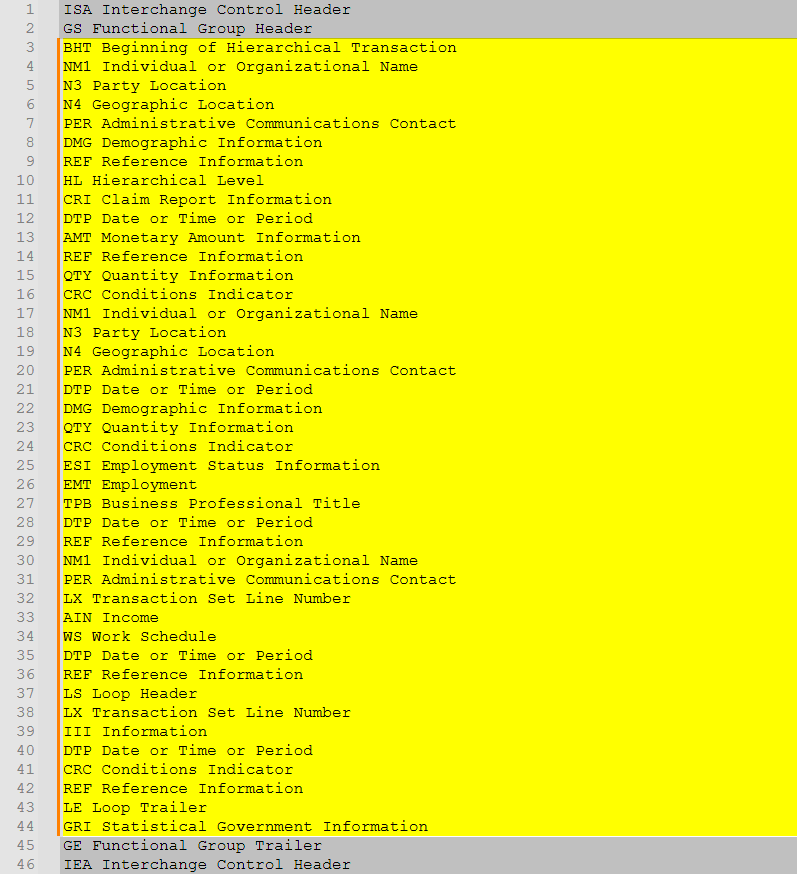
What are the Common Segments Included in the EDI 148 Report of Injury, Illness or Incident?
| Segment | Name | Functional Role |
|---|---|---|
| ST | Transaction Set Header | Identifies the start of the transaction |
| BHT | Beginning of Hierarchical Transaction | Communicates purpose and action |
| NM1 | Individual or Organizational Name | Identifies involved parties |
| HL | Hierarchical Level | Establishes hierarchy |
| CRI | Claim Report Information | Reports incident context |
| DTP | Date or Time or Period | Specifies relevant dates |
| CRC | Conditions Indicator | Indicates conditional attributes |
| SE | Transaction Set Trailer | Identifies transaction end |
What Status Codes are used with the EDI 148?
| Code Type | Description | Usage Context |
|---|---|---|
| Action Codes | Initial, Update, Replace | Indicate reporting intent |
| Condition Codes | Yes / No Indicators | Describe incident conditions |
What Reason Codes are used with the EDI 148 Report of Injury, Illness or Incident?
| Reason Code Category | Description | Business Meaning |
|---|---|---|
| Update Reasons | Data correction or change | Explains resubmission |
| Regulatory Reasons | Jurisdictional requirement | Supports compliance |
What Use Cases does the EDI 148 support?
The EDI 148 supports a range of operational, regulatory, and analytical use cases across workers’ compensation and insurance ecosystems including the First Report of Injury (FROI), Incident Updates, Claims Initiation, and more.
| Use Case | Description | Primary Stakeholders |
|---|---|---|
| First Report of Injury (FROI) | Initial notification of a workplace injury or illness | Employers, Insurers, State Agencies |
| Incident Updates | Submission of corrected or changed incident data | MCOs, TPAs, Insurers |
| Claims Initiation | Triggering of workers’ compensation claim workflows | Insurers, Claims Adjusters |
| Regulatory Reporting | Compliance with state-mandated injury reporting | State Workers’ Compensation Boards |
| Data Synchronization | Ongoing alignment of claim data across systems | Employers, TPAs, Agencies |
What are the Benefits of the EDI 148 Report of Injury, Illness or Incident?
The EDI 148 delivers measurable business and operational benefits by standardizing injury and incident reporting. Benefits include improved data accuracy, reduced manual processing, faster claims initiation, and enhanced regulatory compliance.
| Benefit | Description | Business Impact |
|---|---|---|
| Standardization | Uses a common ANSI X12 format | Reduces ambiguity and errors |
| Automation | Eliminates manual data entry | Improves processing speed |
| Accuracy | Enforces structured data capture | Improves data quality |
| Compliance | Aligns with regulatory requirements | Reduces compliance risk |
| Visibility | Provides timely incident data | Improves decision-making |
How efficient is the EDI 148? 
The EDI 148 Report of Injury, Illness or Incident delivers efficiency gains similar in nature to those achieved by transactional messages such as the EDI 850 Purchase Order or EDIFACT ORDERS, where automation through standardized EDI exchange improves reporting speed, reduces rework, and accelerates downstream processing although applied to injury and incident reporting rather than commercial ordering.
In a manual reporting process, workplace injuries or illnesses are often documented on paper or web forms, rekeyed into internal systems, transmitted via fax, email, or portal uploads, and then manually reviewed, validated, and re-entered by insurers, managed care organizations, or state agencies. Each handoff introduces delay, transcription risk, and the potential need for follow-up clarification before a claim can be initiated, the EDI 148 replaces these fragmented steps with a single, structured electronic transaction.
Once  an injury or incident is recorded (once) in the employer’s or provider’s system, the EDI 148 can be generated and transmitted automatically. The transaction reaches the receiving insurer or regulatory agency in a standardized format that aligns directly with the claim and case management systems of the recipient, eliminating redundant data entry and significantly reducing cycle time, which are very important when it comes to a workplace injury and the potential loss of income.
an injury or incident is recorded (once) in the employer’s or provider’s system, the EDI 148 can be generated and transmitted automatically. The transaction reaches the receiving insurer or regulatory agency in a standardized format that aligns directly with the claim and case management systems of the recipient, eliminating redundant data entry and significantly reducing cycle time, which are very important when it comes to a workplace injury and the potential loss of income.
Efficiency gains become more pronounced in the downstream processing that takes place next. Automated receipt and acknowledgments through the EDI 997 (Functional Acknowledgement) and other control documents confirm technical acceptance almost instantly. Claims systems can then evaluate the incident data, establish a claim record, and trigger eligibility verification or medical management workflows without waiting for manual (human) intervention. When updates are required, the same mechanism (the EDI 148) supports rapid resubmission or synchronization, avoiding delays common in a manual processes.
| Process Area | Manual Reporting | EDI 148 Reporting |
|---|---|---|
| Incident Submission | Paper, fax, email, or portal entry | Automated system-to-system transmission |
| Data Entry | Multiple rekeying steps | Single point of data capture |
| Validation | Manual review | Automated rules and acknowledgments |
| Confirmation | Phone or email follow-up | Immediate EDI 997 acknowledgment |
| Claim Initiation | Delayed and sequential | Near real-time and parallel |
Collapsing multiple manual tasks into a single automated exchange, the EDI 148 enables near real-time incident reporting and faster claim initiation than manual processing. When transactions are free from errors (no errors are detected), the transaction moves directly into downstream claims workflows, allowing insurers and agencies to act on the reported injury or illness almost immediately after submission and without human intervention.
How Compliant is the EDI 148 Report of Injury, Illness or Incident?
The EDI 148 transaction aligns with ANSI ASC X12 standards and supports jurisdiction-specific implementation guides, including state workers’ compensation requirements.
 The Report of Injury, Illness or Incident was designed not only to meet requirements for workers’ compensation partners, they were in fact partners to their creation and maintenance of them. Consortium-driven X12 standards were intentionally designed as open, consensus-based standards, governed by consortiums that represent equally:
The Report of Injury, Illness or Incident was designed not only to meet requirements for workers’ compensation partners, they were in fact partners to their creation and maintenance of them. Consortium-driven X12 standards were intentionally designed as open, consensus-based standards, governed by consortiums that represent equally:
- Employers
- Insurance Carriers and Industry associations
- State agencies and Third-party administrators (TPAs)
- Government and regulatory bodies
- Technology vendors
What is the Format of the EDI 148?
The EDI 148 uses a hierarchical ANSI X12 format within Functional Group IJ, employing standardized segments, elements, and qualifiers. ANSI ASC X12 functional group IJ is assigned to Workers’ Compensation, Claims, and Injury Reporting transactions.
How Accurate is the EDI 148 Report of Injury, Illness or Incident?
EDI 148 Report of Injury, Illness or Incident messages standardize data exchanges and ensure consistent data. These messages standardize the exchange of data between parties which improve accuracy through data structures that ensure visibility, consistency, and facilitate an exchange of critical information between employers, insurance carriers, third-party administrators (TPAs), and state agencies.
Accuracy, as with most data exchanges between and among parties depends on adherence to implementation guidelines, the correct use of qualifiers, and timely updates when incident data changes.
What are the Limitations of the EDI 148?
Limitations include jurisdictional variation, dependency on source data, accurate of incident reporting techniques and complementary transactions which might be necessary to complete claims workflows.
Are Guidelines and Sample Files available for the EDI 148?
Yes. Sample EDI 148 Report of Injury, Illness or Incident implementation guides that support testing and partner onboarding are available through PartnerLinQ. ![]()
Sample EDI 148 implementation guides illustrate both inbound and outbound flows, segment layouts, and valid data examples and support testing and partner onboarding. Customized specification documents for use in on boarding and technical development are available upon request.
PartnerLinQ provides:
- EDI 148 Report of Injury, Illness or Incident implementation guide
- Sample payloads
- Qualification and testing maps
- Error handling and best-practice notes
What are the Basic Questions for EDI Integration with the EDI 148?
The following questions frame the technical, operational, and governance considerations that typically arise when integrating the EDI 148 Report of Injury, Illness or Incident. These questions reflect patterns consistently observed across recent PartnerLinQ transaction documents.
| Integration Question | What to Evaluate | Why It Matters |
|---|---|---|
| Are samples and specifications available? | Availability of X12 base specs and jurisdiction-specific implementation guides | Reduces interpretation risk and accelerates onboarding |
| What is the general direction of the transaction? | Whether the 148 is sent outbound or received inbound by the organization | Determines system ownership and flow design |
| Is the transaction inbound or outbound? | Role-based behavior across employers, MCOs, TPAs, and agencies | Drives mapping, validation, and monitoring strategy |
| What response to the transaction is expected or sent? | Requirement for an EDI 997 Functional Acknowledgment | Confirms receipt and syntactic compliance |
| Are response samples and specifications available? | Access to 997 samples or downstream response formats | Supports testing and exception handling |
| Are there other interested parties? | Identification of TPAs, MCOs, regulators, or analytics platforms | Expands coordination and governance scope |
| What transactions might these parties participate in? | Use of 270, 271, 837P, and related transactions | Enables end-to-end workflow planning |
| How are changes to the EDI 148 handled today? | Full resubmission versus partial update rules | Impacts versioning and data stewardship |
| Is the transaction triggered automatically or manually? | System events versus human initiation | Defines automation opportunities |
| Are responses and updates automatically triggered? | Automated updates versus manual intervention | Influences SLAs and operational workload |
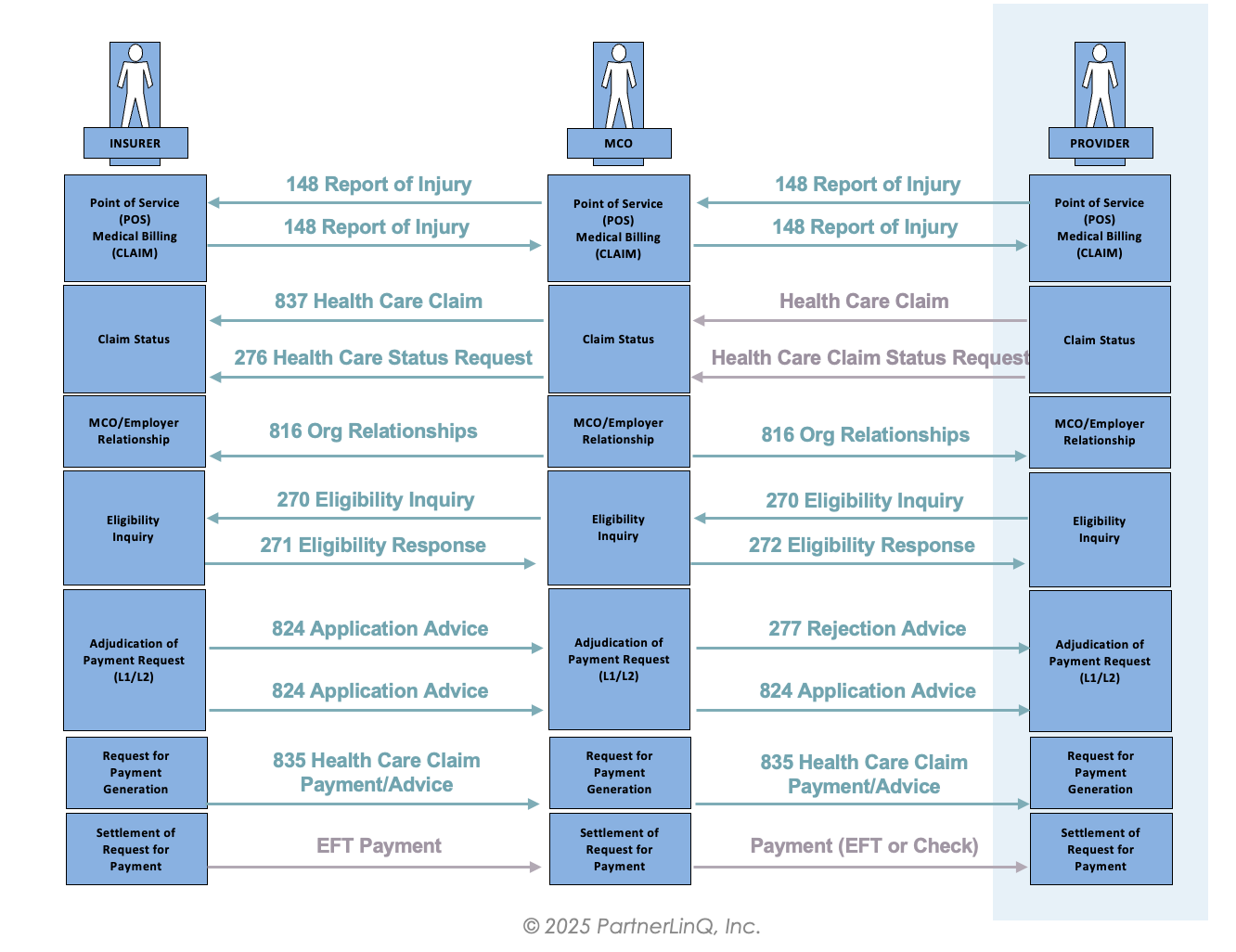
What Business Level Workflow does the EDI 148 support?
The EDI 148 transaction supports workers’ compensation reporting workflows from incident occurrence extending through claim establishment, eligibility verification, and downstream medical and regulatory processes.
Business-Level Workflow Overview
- Incident Occurs - A workplace injury, illness, or incident is identified by an employer or healthcare provider.
- Incident Recorded in Source System - The incident is captured in an HR, safety, clinical, or case-management system with employee, employer, and incident details.
- EDI 148 Generated and Transmitted - The source system generates an EDI 148 and transmits it to the insurer, managed care organization (MCO), or state agency.
- Acknowledgment and Validation - The receiving party validates the transaction and returns an EDI 997 Functional Acknowledgment, confirming technical acceptance.
- Claim Initiation and Case Creation - Claims systems automatically create or update a workers’ compensation claim based on the reported incident.
- Eligibility and Coverage Verification - The EDI 148 may be followed by EDI 270/271 exchanges to confirm coverage and benefits.
- Medical and Benefit Processing - Once eligibility is confirmed, medical treatment and benefit workflows proceed, often involving EDI 837P claims.
Ongoing Updates and Synchronization - Subsequent EDI 148 transactions communicate changes such as updated injury details, provider changes, or employment status updates.
What are the Best Practices for using the EDI 148?
Effective use of the EDI 148 depends on disciplined governance, consistent data quality controls, and alignment with jurisdictional implementation guidance.
| Best Practice | Description | Operational Benefit |
|---|---|---|
| Validate data prior to transmission | Perform syntactic and business-rule validation before sending | Reduces rejections and rework |
| Follow jurisdiction-specific rules | Apply state or agency implementation requirements | Ensures regulatory compliance |
| Use consistent qualifiers and codes | Standardize code usage across submissions | Improves downstream interpretation |
| Automate incident triggers | Generate 148 transactions from system events | Improves timeliness |
| Manage updates carefully | Resend complete business sets when required | Preserves data integrity |
| Monitor acknowledgments | Track 997 responses and errors | Improves operational visibility |
What Transactions are associated with the EDI 148?
| Transaction | Description |
|---|---|
| 997 | Functional Acknowledgment |
| 270 | Eligibility Inquiry |
| 271 | Eligibility Response |
| 837P | Professional Health Care Claim |
Footnotes
- PartnerLinQ EDI Implementation Guidance for Transaction Set 148.
- Ohio Bureau of Workers’ Compensation EDI Reporting Requirements (Implementation Guidance for Transaction Set 148)
Explore Our Integration Solutions
PartnerLinQ Integration Solutions
Connect Everything. Integrate Intelligently.
Future-Proof Your Business with Composable, AI Powered Connectivity.



