 What is the EDI 270?
What is the EDI 270?
The EDI 270 is a HIPAA-standard electronic transaction used by healthcare providers to request patient eligibility, coverage, and benefit information from a payer. It enables real-time or batch verification of insurance status, helping reduce claim denials and improve upfront financial accuracy before services are rendered.
Transaction Identity Block
| Attribute | Value |
|---|---|
| Transaction Name | Eligibility, Coverage, or Benefit Inquiry |
| X12 Transaction Set | 270 |
| Functional Group | HS |
| Industry Usage | Healthcare, Insurance, Government |
| Primary Purpose | Verify eligibility and benefits |
| Typical Sender | Healthcare Provider / Clearinghouse |
| Typical Receiver | Insurance Payer |
| Common Preceding Transactions | Patient Registration |
| Common Following Transactions | 271, 837 |
| Standard Version | X12 005010X279A1 |
How does PartnerLinQ use the X12 EDI 270 – Eligibility, Coverage, or Benefit Inquiry?
PartnerLinQ  uses the EDI 270 to enable healthcare providers, insurers, managed care organizations, and other authorized entities to request information about a patient's eligibility, benefits, or coverage under a health plan, typically prior to delivering services. Healthcare providers, insurers, and other authorized entities typically send an EDI 270 inquiry to the payer (insurance company, government agency, etc.) requesting coverage details. The payer (insurance company, government agency, etc.) then responds with an EDI 271 Eligibility, Coverage, or Benefit Response, to providers, insurers, and other authorized entities with the requested information. The EDI 270 transaction supports HIPAA-compliant inquiries and integrates directly with payer systems to reduce manual outreach such as phone calls, faxes, and emails, improving operational efficiency and data accuracy.
uses the EDI 270 to enable healthcare providers, insurers, managed care organizations, and other authorized entities to request information about a patient's eligibility, benefits, or coverage under a health plan, typically prior to delivering services. Healthcare providers, insurers, and other authorized entities typically send an EDI 270 inquiry to the payer (insurance company, government agency, etc.) requesting coverage details. The payer (insurance company, government agency, etc.) then responds with an EDI 271 Eligibility, Coverage, or Benefit Response, to providers, insurers, and other authorized entities with the requested information. The EDI 270 transaction supports HIPAA-compliant inquiries and integrates directly with payer systems to reduce manual outreach such as phone calls, faxes, and emails, improving operational efficiency and data accuracy.
What responses to the EDI 270 are expected or sent?
The EDI 270 – Eligibility, Coverage, or Benefit Inquiry is paired with the EDI 271 Eligibility, Coverage, or Benefit Response. Upon receipt of a valid inquiry, the payer responds with an EDI 271 containing eligibility status, coverage details, and benefit information. A functional acknowledgment (EDI 997) may also be returned to confirm syntactic receipt. The Functional Acknowledgment (997) is an ANSI X12 EDI transaction set that represents industry best practice and is automatically generated by modern EDI software. It confirms delivery and receipt of information, validates syntax, and reports any formatting errors or data loss. Unlike a Message Delivery Notification (MDN), which only confirms transport-level delivery, the 997 provides feedback on the structural integrity of the message. Business documents may be accepted with errors or rejected outright, with rejected messages requiring correction and re-transmission by the sender. By providing this level of detail, the 997 ensures that corrected transactions are properly structured and ready for downstream processing.
EDI 270 – Eligibility, Coverage, or Benefit Inquiry is paired with the EDI 271 Eligibility, Coverage, or Benefit Response. Upon receipt of a valid inquiry, the payer responds with an EDI 271 containing eligibility status, coverage details, and benefit information. A functional acknowledgment (EDI 997) may also be returned to confirm syntactic receipt. The Functional Acknowledgment (997) is an ANSI X12 EDI transaction set that represents industry best practice and is automatically generated by modern EDI software. It confirms delivery and receipt of information, validates syntax, and reports any formatting errors or data loss. Unlike a Message Delivery Notification (MDN), which only confirms transport-level delivery, the 997 provides feedback on the structural integrity of the message. Business documents may be accepted with errors or rejected outright, with rejected messages requiring correction and re-transmission by the sender. By providing this level of detail, the 997 ensures that corrected transactions are properly structured and ready for downstream processing.
What does the EDI 270 – Eligibility, Coverage, or Benefit Inquiry support?
The EDI 270 supports eligibility verification, coverage confirmation, benefit inquiry, and coordination of benefits. The transaction enables organizations to validate coverage prior to treatment, reducing claim denials and rework.
What is EDI 270 used for?
The EDI 270 is used to verify whether a patient is eligible for insurance coverage and to determine what benefits apply for specific services. It is typically sent before treatment to confirm coverage, copayments, deductibles, and service limitations, reducing administrative work and preventing billing errors.
Who uses the EDI 270?
The  EDI 270 is used by healthcare providers, hospitals, clinics, billing companies, and clearinghouses to request eligibility and benefit information from insurance payers. Health plans, government agencies, and managed care organizations receive the inquiry and respond with an EDI 271 transaction.
EDI 270 is used by healthcare providers, hospitals, clinics, billing companies, and clearinghouses to request eligibility and benefit information from insurance payers. Health plans, government agencies, and managed care organizations receive the inquiry and respond with an EDI 271 transaction.
When Is the EDI 270 Required?
A requirement codified in federal regulation 45 CFR § 162.1202 – The U.S. Department of Health and Human Services (HHS) adopted the EDI 270/271 as a national standard for eligibility for a health plan transactions.
Implemented and enforced through the Centers for Medicare & Medicaid Services (CMS) The ASC X12N EDI 270 is the standard for Eligibility for a health plan inquiry and the ASC X12N EDI 271 is the standard for eligibility for a health plan response 
While a dependency on an EDI Infrastructures exists, one that requires all parties to have compatible EDI systems, compliance is achieved and reinforced through implementation guides, paired-response requirements with the EDI 271, and the use of standardized qualifiers and codes within the EDI 270/271 exchange. Organizations that adhere to the guidelines and derivative documents like this one benefit from expanded use, predictable responses and reduced downstream exceptions.
Is the EDI 270 Mandated Under Regulation?
The EDI 270/271 transactions are part of the HIPAA Administrative Simplification standards, which require covered entities to use adopted electronic formats for eligibility inquiries. These standards ensure consistent data exchange across healthcare providers, payers, and clearinghouses, as defined by federal regulation and enforced nationally.
How Does the EDI 270 Work in the Business Workflow?
The EDI 270 works by allowing a healthcare provider to send an electronic eligibility inquiry to a payer before services are delivered. The payer evaluates coverage and returns an EDI 271 response with eligibility status and benefit details, enabling providers to confirm coverage, estimate costs, and reduce claim denials.
Upstream Transactions
| Transaction | Purpose |
|---|---|
| Patient Registration | Captures demographic and insurance data |
| Scheduling | Triggers eligibility verification |
Downstream Transactions
| Transaction | Purpose |
|---|---|
| 271 | Returns eligibility response |
| 837 | Submits claim |
| 835 | Processes payment |
End-to-End Workflow Example
A patient schedules an appointment, triggering an automated EDI 270 eligibility inquiry from the provider system to the payer. The payer evaluates coverage and returns an EDI 271 response with eligibility status and benefit details. The provider uses this information to confirm services, estimate patient responsibility, and proceed with care, ensuring accurate billing and reduced claim denials.
When is the EDI 270 sent?
The EDI 270 is typically sent during appointment scheduling, pre-registration, or patient check-in. It may also be re-sent prior to high-cost procedures or when coverage may have changed, ensuring accurate eligibility verification before services are rendered.
What are the Key Features of the healthcare eligibility EDI 270?
Key features evolve around who is covered, what is covered, and under what conditions, It include standardized eligibility inquiry, hierarchical party identification, traceability through unique reference numbers, and direct pairing with the EDI 271 response and is a HIPAA-compliant healthcare transaction. The transaction supports multiple lines of insurance and jurisdictional-specific implementations allowing for inquiries at multiple levels:
- Subscriber
- Dependent
- Plan
- Service category (CPT/HCPCS groupings)
The EDI 270 – Eligibility, Coverage, or Benefit Inquiry is always paired with the EDI 271 (Eligibility Response), forming a request/response transaction set perfect for systemic automation, together, they enable automated eligibility confirmation and benefit explanation.
What is the Purpose of the EDI 270 – Eligibility, Coverage, or Benefit Inquiry?
The purpose of the EDI 270 Eligibility, Coverage, or Benefit Inquiry is to provide a reliable, standardized, and auditable mechanism for determining whether an individual is eligible for coverage and what benefits apply at a specific point in time.
In practical terms, the EDI 270 initiates a lifecycle by establishing shared understanding and certainty much like the EDI 850 Purchase Order fulfills in order management, the EDI 270 enables organizations to proceed with confidence, accuracy, and speed.
What Information is Included in the EDI X12 270 format?
The  transaction includes payer, provider, subscriber, and dependent identification, demographic information, reference identifiers, relevant dates, and the specific type of eligibility or benefit being requested.
transaction includes payer, provider, subscriber, and dependent identification, demographic information, reference identifiers, relevant dates, and the specific type of eligibility or benefit being requested.
- Patient and Subscriber Information
- Payer Information
- Provider Information
- Inquiry Type (Coverage vs. Benefits)
- Service Type / Service Category
- Date or Date Range of Service
- Plan and Coverage Context
- Request for Additional Benefit Details (Optional)
| Segment | Name | What It Contains | Business Purpose |
|---|---|---|---|
| BHT | Beginning of Hierarchical Transaction | Purpose code, reference number, transaction date/time | Identifies the inquiry purpose (original, re-submission) |
| NM1 | Individual or Organizational Name | (1, 2) Payer, Provider, Subscriber, or Patient name + ID | Identifies each party in the transaction |
| REF | Reference Identification | Payer ID, Provider Tax ID, or plan reference | Supports trading partner and plan identification |
| PRV | (3) Provider Information | Provider specialty or taxonomy | Used for benefit rules tied to provider type |
| INS | Insured Benefit | Relationship to subscriber (self, spouse, child) | Defines who is being checked |
| DTP | Date or Time Period | (6) Date of service or coverage date | Determines if coverage is active |
| EQ | Eligibility or Benefit Inquiry | (5, 7) Service Type Code(s) (e.g., medical, dental, mental health) | Defines what benefits are being requested |
| AMT | Monetary Amount | Requested deductible or benefit amount | Supports financial benefit queries |
| III | Additional Inquiry Information | Coverage level or insurance type | (4, 8) Adds refinement to benefit inquiry (Coverage vs. Benefits) |
What are the Essential Components of the EDI 270 – Eligibility, Coverage, or Benefit Inquiry?
| Component Category | Description | Business Purpose |
|---|---|---|
| Transaction Control | ST / SE segments | Define transaction boundaries |
| Hierarchical Structure | BHT / HL segments | Establish inquiry context |
| Party Identification | NM1 / REF / DMG | Identify payer, provider, subscriber |
| Traceability | TRN | Correlate inquiry and response |
| Inquiry Detail | EQ | Specify benefit or coverage requested |
What are the Common Segments Included in the X12 270 format?
The EDI 270 includes key segments such as ST (transaction header), BHT (purpose), HL (hierarchy), NM1 (party identification), DMG (demographics), DTP (dates), and EQ (eligibility inquiry). These segments work together to define the patient, provider, payer, and the specific benefits being requested.
| Segment | Name | Functional Role |
|---|---|---|
| ST | Transaction Set Header | Begins the transaction |
| BHT | Beginning of Hierarchical Transaction | Defines inquiry purpose |
| HL | Hierarchical Level | Organizes inquiry levels |
| TRN | Trace | Correlates 270 and 271 |
| NM1 | Individual or Organizational Name | Identifies parties |
| REF | Reference Information | Supplies identifiers |
| DMG | Demographic Information | Identifies the individual |
| DTP | Date or Time or Period | Specifies coverage dates |
| EQ | Eligibility or Benefit Inquiry | Identifies requested information |
| SE | Transaction Set Trailer | Ends the transaction |
Summary Table of Key Segments
| Segment | Primary Use |
|---|---|
| ST | Transaction identification |
| BHT | Inquiry intent and timing |
| HL | Structural hierarchy |
| TRN | Inquiry traceability |
What Status Codes are used with the EDI 270 – Eligibility, Coverage, or Benefit Inquiry?
Unlike  claim or advice transactions, the EDI 270 does not approve or deny services, it serves as a request as to the type of eligibility or benefit and how the inquiry document should be interpreted by the receiving payer.
claim or advice transactions, the EDI 270 does not approve or deny services, it serves as a request as to the type of eligibility or benefit and how the inquiry document should be interpreted by the receiving payer.
Status-related indicators within the EDI 270 appear mostly through purpose codes, service type codes, and hierarchical qualifiers, which together define the scope and intent of the inquiry, codes that ensure that the responding EDI 271 can return accurate, relevant, and properly contextualized benefit information.
| Status Code Category | Where Used | Description | Business Purpose |
|---|---|---|---|
| Transaction Set Purpose Code | BHT02 | Identifies the inquiry as a request | Signals that eligibility or benefit information is being requested |
| Hierarchical Level Codes | HL03 | Identifies information source, receiver, subscriber, or dependent | Establishes inquiry context |
| Service Type Codes | EQ01 | Identifies the category of benefits being requested | Scopes the 271 response content |
| Trace Type Codes | TRN01 | Identifies the transaction trace context | Enables inquiry-response correlation |
These status-related codes ensure that eligibility inquiries are processed consistently and routed correctly within payer systems. When used correctly, they eliminate ambiguity and reduce the likelihood of incomplete or mismatched responses.
What Reason Codes are used with the EDI X12 270 format?
The EDI 270 enables payers to respond with precise eligibility and benefit information by clearly distinguishing intent (status) from context (reason)and maintaining predictable, standards-based processing. A separation that mirrors the design philosophy used in the EDI 148, where action and reason are conveyed through structured qualifiers rather than free-form (text) interpretation.
| Reason Category | Description | Business Meaning |
|---|---|---|
| Coverage Inquiry Reasons | Benefit or coverage clarification | Support decision-making |
Reason codes associated with the EDI 270 address why eligibility or benefit information is being requested, codes that guide the payer in determining data to return in the EDI 271 response.
| Reason Code Category | Where Used | Description | Business Meaning |
|---|---|---|---|
| Service Classification Codes | EQ01 | Identifies the type of benefit being inquired upon | Explains why coverage data is requested |
| Reference Qualifiers | REF01 | Identifies external identifiers such as policy numbers | Links inquiry to a specific coverage context |
| Date Qualifiers | DTP01 | Identifies plan or coverage date ranges | Explains timing relevance of the inquiry |
What Use Cases does the EDI 270 message support?
The EDI 270 supports a broad range of operational, clinical, and administrative use cases by enabling real-time access to eligibility, coverage, and benefit information prior to the delivery of services. These use cases mirror the role the EDI 148 plays in incident reporting, but apply upstream in the care and claims lifecycle where coverage certainty is critical.
| Use Case | Description | Stakeholders |
|---|---|---|
| Eligibility Verification | Confirms whether an individual is actively covered under a plan | Providers, Insurers, MCOs |
| Coverage Validation | Determines what services are covered or excluded | Providers, Claims Teams |
| Benefit Inquiry | Verifies copayments, deductibles, coinsurance, and limits | Providers, Members |
| Coordination of Benefits (COB) | Identifies multiple plans and payment order | Insurers, TPAs |
| Pre-Service Validation | Confirms coverage before treatment | Providers, Patients |
What are the Benefits of the healthcare eligibility EDI 270 transaction message?
The EDI 270 delivers business and operational benefits by standardizing eligibility and benefit inquiries across payers and jurisdictions. The EDI 270 and 271 response determine if coverage is active, defines what benefits are being requested, and supports financial benefit queries that improve outcomes that include patient-care.
| Benefit | Description | Business Impact |
|---|---|---|
| Standardization | Uses a common ANSI X12 format | Reduces interpretation errors |
| Automation | Reduces manual inquiries, replacing phone, fax, email, and portal checks | Accelerates verification |
| Accuracy | Uses structured data and standard identifiers | Reduces claim denials |
| Compliance | Aligns with HIPAA and payer rules | Lowers regulatory risk |
| Visibility | Provides timely coverage insight | Improves decision-making |
| Timeliness | Automation delivers near real-time responses | Improved patient experience |
How efficient is the EDI 270 – Eligibility, Coverage, or Benefit Inquiry?
The EDI 270 replaces manual eligibility verification methods such as phone, fax, email, and portal inquiries with a single automated electronic inquiry and can be processed in real-time or batch mode. Real-time inquiries are used during patient check-in for immediate eligibility verification, while batch processing is used for pre-visit validation at scale. Both approaches improve efficiency and reduce manual eligibility verification efforts.
EDI 270 replaces manual eligibility verification methods such as phone, fax, email, and portal inquiries with a single automated electronic inquiry and can be processed in real-time or batch mode. Real-time inquiries are used during patient check-in for immediate eligibility verification, while batch processing is used for pre-visit validation at scale. Both approaches improve efficiency and reduce manual eligibility verification efforts.
Once transmitted, the inquiry (EDI 270), a model of efficiency, is processed electronically. Results of the inquiry (EDI 270) is returned via the EDI 271 (Eligibility, Coverage or Benefit Information), thus enabling a rapid confirmation of coverage and benefits before services are rendered, improving decision-making, improving the patient experience while reducing claim denials.
Is the EDI 270 required by HIPAA?
Yes. The EDI 270 is mandated under HIPAA Administrative Simplification Rules as the standard format for electronic eligibility inquiries. The requirement is defined by the U.S. Department of Health and Human Services and codified in 45 CFR § 162.1202, ensuring nationwide interoperability.
How Compliant is the EDI 270?
The EDI 270 aligns with ANSI ASC X12 standards and is a core HIPAA-mandated transaction for eligibility, coverage, and benefit inquiry. The transaction was developed through a consortium-driven standards process involving healthcare providers, insurers, government agencies, and technology vendors, ensuring broad industry adoption and regulatory alignment.
What is the difference between EDI 270 and EDI 271?
The EDI 270 is an eligibility inquiry sent by providers to request coverage and benefit information, while the EDI 271 is the payer’s response containing eligibility status, coverage details, and financial responsibility. Together, they form a request-response pair used for automated insurance verification.
| Feature | EDI 270 | EDI 271 |
|---|---|---|
| Type | Inquiry | Response |
| Sender | Provider | Payer |
| Purpose | Request eligibility | Return benefits |
| Timing | Pre-service | Real-time response |
What is the Format of the EDI 270 – Eligibility, Coverage, or Benefit Inquiry?
The EDI 270 uses a hierarchical ANSI X12N format transmitted within Functional Group HS. The transaction employs standardized segments, loops, and qualifiers to identify information sources, receivers, subscribers, and dependents. A structured format that ensures consistent interpretation and reliable pairing with the corresponding EDI 271 response.
How Accurate is the EDI 270? 
Accuracy depends on precise party identification including specific patient identification (name, DOB, HICN or MBI), precise eligibility or benefit information (EB) and service type (EB03) in order to properly identify health benefit plan coverage eligibility. An accurate response depends use of valid reference numbers, adherence to implementation guidelines, standards, and the ability to identify and react to coded responses found within the EDI 271 such as might be found in the AAA03 Reject Reason Code and AAA04 Follow-up Action Code which electronically communicate issues with the 270 request that might require attention.
What are the Limitations of the EDI 270?
Limitations include reliance on source data, data quality and jurisdiction-specific constraints that may limit the benefit detail available in an automated response.
Does EDI 270 Guarantee Payment?
No. The EDI 270/271 process verifies eligibility and benefits but does not guarantee payment. Final payment depends on claim submission accuracy, medical necessity, authorization requirements, and payer adjudication rules.
Are Implementation Guidelines and Sample Files Available for the EDI 270?
Yes. PartnerLinQ provides sample transactions and implementation guides. EDI 270 implementation guides illustrate both inbound and outbound flows, segment layouts, and valid data examples and support testing and partner onboarding.
Companion Guides
Trading partners frequently publish EDI 270 implementation guidelines defining segment usage and validation rules. Customized specification documents for use in on boarding and technical development are available through PartnerLinQ Support and Guideline Management.
Trading Partner Requirements
 Customized mapping, testing, and validation documentation are also available. Partners may specify:
Customized mapping, testing, and validation documentation are also available. Partners may specify:
- Mapping
- Identifier use (standards)
- Validation rules
- Response rules
EDI 270 Example File (X12 Sample)
BHT*0022*13*10001234*20240101*1319~
HL*1**20*1~
NM1*PR*2*INSURANCE COMPANY*****PI*12345~
HL*2*1*21*1~
NM1*1P*2*PROVIDER NAME*****XX*1234567890~
HL*3*2*22*0~
NM1*IL*1*DOE*JOHN****MI*ABC123456~
DMG*D8*19800101*M~
DTP*291*D8*20240101~
EQ*30~
SE*10*0001~
EDI 270 Example File (Annoted)
| Segment | Meaning | Business Context |
|---|---|---|
| ST | Transaction Start | Begins eligibility inquiry |
| BHT | Transaction Purpose | Defines request type |
| HL | Hierarchy | Structures payer → provider → subscriber |
| NM1*PR | Payer | Insurance company |
| NM1*1P | Provider | Requesting entity |
| NM1*IL | Subscriber | Patient |
| DMG | Demographics | DOB / gender |
| DTP | Service Date | Coverage timing |
| EQ*30 | Service Type | Health benefit plan |
Common Errors and Rejection Scenarios
| Error Type | Example | Business Impact |
|---|---|---|
| 999 Rejection | Syntax error | Transaction not processed |
| AAA Reject | Invalid member ID | No eligibility returned |
| Missing DOB | Patient not found | Delayed verification |
| Invalid Service Code | EQ mismatch | Incorrect benefits returned |
What are the Basic Questions for EDI Integration with the EDI 270?
| Integration Question | What to Evaluate | Why It Matters |
|---|---|---|
| Are samples and implementation guides available? | Availability of X12 base specifications and payer- or jurisdiction-specific 270 guides | Accelerates onboarding and reduces interpretation risk |
| What is the general direction of the transaction? | Outbound inquiry from provider, employer, or intermediary | Defines system roles and routing logic |
| Is the transaction inbound or outbound? | Role-based behavior across providers, insurers, and agencies | Drives mapping, validation, and monitoring strategy |
| What response to the transaction is expected or sent? | Requirement for an EDI 271 Eligibility Response | Completes the inquiry lifecycle |
| Are response samples and specifications available? | Access to 271 samples and business rules | Improves testing and exception handling |
| Are there other interested parties? | Clearinghouses, TPAs, MCOs, state agencies | Expands coordination and governance scope |
| What transactions might these parties participate in? | 271, 837, 997 | Enables end-to-end workflow planning |
| How are changes or repeat inquiries handled? | Re-inquiry timing versus manual escalation | Impacts operational workload and SLA design |
| Is the transaction triggered automatically or manually? | System events versus user-driven requests | Defines automation opportunities |
| Are inquiries and responses automatically processed? | Automated consumption of 271 responses | Improves processing velocity and decision support |
| Are jurisdiction-specific rules enforced? | State or payer constraints on inquiry content | Prevents misinterpretation and compliance issues |
The following questions frame the technical, operational, and governance considerations commonly encountered when integrating the EDI 270 Eligibility, Coverage, or Benefit Inquiry.
What Business Level Workflow does the EDI 270 support?
The EDI 270 supports pre-service eligibility verification workflows that ensure coverage and benefit information is known before treatment or claim submission.
| Business Stage | Business Purpose |
|---|---|
| Appointment Scheduling / Registration | Patient schedules visit or checks in which triggers need to verify insurance |
| Eligibility Inquiry | Provider system eligibility request is routed to the correct payer system confirming if patient is covered and what benefits apply |
| Eligibility Response & Adjudication | Payer matches member, determines coverage and benefit applicability, returns a structured response (271) providing coverage status and benefit details |
| Financial & Clinical Decision making | Supports patient estimates and care planning (Example: Dental care) |
| Downstream Revenue Cycle | Claim and payment processing using verified data, reducing rejections and rework |
What are the Best Practices for using the EDI 270 ?
Used properly, the EDI 270 shifts eligibility, payment, and collections from reactive to predictable, automated business process that reduce denials and improves financial transparency for patients and providers. The EDI 270 is most effective when it is targeted to specific services, integrated into front-end revenue cycles and workflows, paired with automation (EDI 270/271 cycle processing), and governed by companion guides.
| Best Practice | Description | Benefit |
|---|---|---|
| Use Automation | Integrate 270/271 directly with Appointment, PMS (Practice Management System) and EHR (Electronic Health Record) workflows | Streamlines administrative, financial, and clinical workflows. Eliminates manual eligibility lookups and re-keying |
| Identify/Match/Validate Patient Identification | Always include the most complete patient information (Member ID, DOB, name, relationship code). Validate files against implementation guidance | Catches structural errors before transmission, reduces mismatches and “unable to identify member” responses |
| Identify/Match Service Codes | Use specific Service Type Codes (not just “general”) when possible | Returns more precise benefit information (copay, deductible, limits) |
| Identify/Match Date of Service | Always include the actual or planned service date (DTP segment) | Ensures coverage is evaluated for the correct time period |
| Identify/Match Provider | Use National Provider Identifier (NPI) taxonomy. Follow payer-specific companion guides | Avoids rejections caused by provider, provider-type or network-dependencies |
| Use Real-Time Inquiry | Send 270 inquiries early and often - Use real-time 270s for check-in and batch 270s for pre-visit verification | Balances operational efficiency with responsiveness and prevents last-minute surprises due to coverage changes |
| Audit & Log Response Handling / Exception Management | Log inquiry/response pairs with timestamps and control numbers. Flag ambiguous or incomplete 271 responses for manual review, process, pair, store, and associate results with patient records | Prevents incorrect billing or patient misinformation, ensures eligibility results are auditable and actionable and supports compliance, troubleshooting, and audits |
| Use in Financial Counseling | Use 270/271 results to generate patient estimates | Improves collections and patient trust |
| Security | Encrypt transmissions and follow HIPAA security rules | Protects PHI and avoids regulatory penalties |
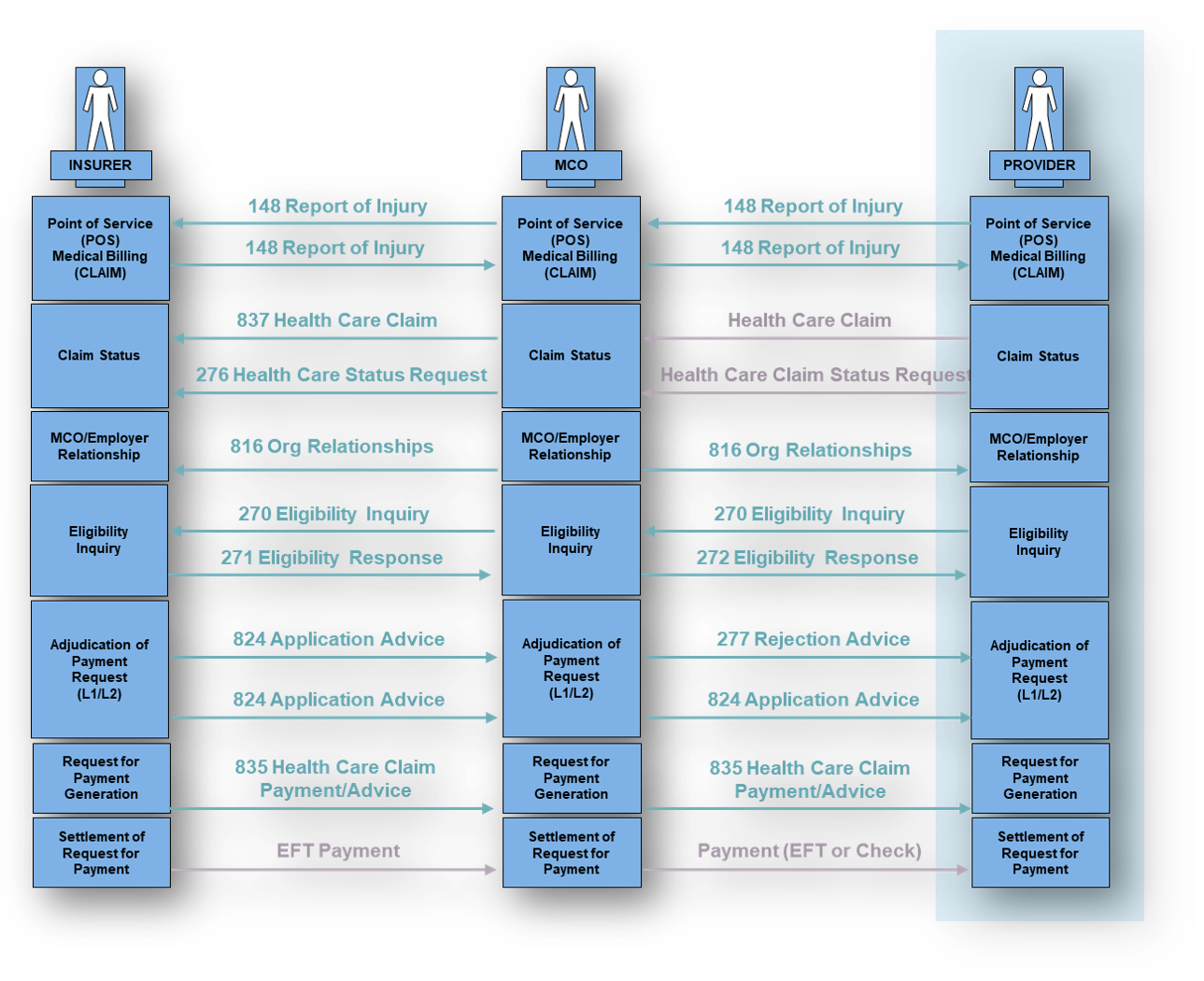
What Transactions are associated with the EDI 270?
| Transaction | Name | Role in the Workflow | Relationship to EDI 270 |
|---|---|---|---|
| 271 | Eligibility, Coverage, or Benefit Information | Returns coverage and benefit details | Direct response to the 270 inquiry |
| 837 | Health Care Claim | Submits a claim for services rendered | Uses eligibility results validated by the 270/271 |
| 835 | Health Care Claim Payment/Advice (ERA) | Provides payment and remittance information | Confirms financial outcome after eligibility was verified |
| 276 | Claim Status Inquiry | Requests claim status | Used if claim processing is delayed after eligibility check |
| 277 | Claim Status Response | Returns claim status | Complements the 276 inquiry |
| 278 | Health Care Services Review (Authorization) | Requests prior authorization | Triggered if 271 shows authorization is required |
| 999 | Implementation Acknowledgment | Confirms syntactical acceptance of the 270 | Verifies the file was structurally valid |
| 997 | Functional Acknowledgment | Confirms receipt of the 270 | Older alternative to the 999 |
| 824 | Application Advice | Reports application-level errors | Sent if business rules fail (e.g., invalid member ID) |
Healthcare Claim Lifecycle Using EDI Transactions
↓
270 Eligibility Inquiry
↓
271 Eligibility Response
↓
837 Health Care Claim
↓
277 Claim Status Response
↓
835 Remittance Advice
What Transactions Are Associated with the EDI 270?
| Transaction | Role |
|---|---|
| 270 | Eligibility Inquiry |
| 271 | Eligibility Response |
| 276 | Claim Status Request |
| 277 | Claim Status Response |
| 824 | Application Advice |
| 835 | Payment / Remittance Advice |
Collectively, the transactions below support the full healthcare claim lifecycle.
Companion Transactions in the Healthcare EDI Workflow
Healthcare claim processing involves several standardized EDI transactions that work together to verify eligibility, submit claims, track status, and process payment.
| Transaction | Name | Role in Workflow |
|---|---|---|
| EDI 270 | Eligibility Inquiry | Checks patient insurance coverage |
| EDI 271 | Eligibility Response | Confirms insurance eligibility |
| EDI 276 | Claim Status Request | Requests claim processing status |
| EDI 277 | Claim Status Response | Returns claim status updates |
| EDI 835 | Health Care Claim Payment/Advice | Communicates reimbursement and remittance details |
| EDI 837 | Health Care Claim | Submits healthcare billing information |
Frequently Asked Questions About the EDI 270
What is EDI 270?
The EDI 270 is a HIPAA-standard electronic transaction used by healthcare providers to request patient eligibility, coverage, and benefit information from a payer. It enables real-time or batch insurance verification, helping reduce claim denials and improve financial accuracy before services are delivered.
What is EDI 270 used for?
The  EDI 270 is used to verify whether a patient has active insurance coverage and to determine what benefits apply to specific services. Providers use it before treatment to confirm eligibility, copayments, deductibles, and service limitations, reducing administrative effort and preventing billing errors.
EDI 270 is used to verify whether a patient has active insurance coverage and to determine what benefits apply to specific services. Providers use it before treatment to confirm eligibility, copayments, deductibles, and service limitations, reducing administrative effort and preventing billing errors.
Who sends the EDI 270 transaction?
Healthcare providers, hospitals, clinics, billing companies, and clearinghouses send the EDI 270 transaction. It is transmitted to insurance payers, managed care organizations, or government agencies to request eligibility and benefit information for a patient prior to delivering services.
Who receives the EDI 270?
Insurance payers, including commercial health plans, government programs, and managed care organizations, receive the EDI 270 transaction. These entities process the inquiry and return an EDI 271 response containing eligibility status, coverage details, and benefit information.
When is the EDI 270 sent?
The EDI 270 is typically sent during appointment scheduling, pre-registration, or patient check-in. It may also be re-sent before high-cost procedures or when coverage changes are suspected, ensuring accurate eligibility verification prior to services being performed.
Is EDI 270 required by HIPAA?
Yes.  The EDI 270 is mandated under HIPAA Administrative Simplification as the standard format for electronic eligibility inquiries. It is defined by the U.S. Department of Health and Human Services and codified in 45 CFR § 162.1202 to ensure nationwide interoperability.
The EDI 270 is mandated under HIPAA Administrative Simplification as the standard format for electronic eligibility inquiries. It is defined by the U.S. Department of Health and Human Services and codified in 45 CFR § 162.1202 to ensure nationwide interoperability.
What is the difference between EDI 270 and EDI 271?
The EDI 270 is an eligibility inquiry sent by providers to request coverage and benefit information, while the EDI 271 is the payer’s response. The 271 returns eligibility status, coverage details, and financial responsibility, forming a request-response pair used for automated insurance verification.
What information is included in an EDI 270?
An EDI 270 includes patient and subscriber identification, provider and payer information, service type codes, and the date of service. It also specifies the type of eligibility or benefit being requested, enabling the payer to return accurate coverage and financial details.
How does the EDI 270 fit into the healthcare workflow?
The EDI 270 is used at the beginning of the revenue cycle to verify eligibility before services are provided. It is followed by the EDI 271 response, and later supports claim submission (837) and payment processing (835), reducing denials and improving billing accuracy.
Does EDI 270 require real-time processing?
No. The EDI 270 supports both real-time and batch processing. Real-time inquiries are used for immediate eligibility verification at check-in, while batch processing allows providers to verify eligibility for multiple patients in advance, improving operational efficiency.
What are common errors in EDI 270 transactions?
Common EDI 270 errors include invalid member IDs, missing demographic data such as date of birth, incorrect service type codes, and syntax errors that trigger 999 or AAA rejections. These issues can delay eligibility verification and require correction before resubmission.
What happens if an EDI 270 is rejected?
If an EDI 270 is rejected, the payer or clearinghouse returns an error such as a 999 or AAA rejection code. The provider must correct the issue, such as invalid member information or formatting errors, and resubmit the transaction to obtain eligibility results.
Footnotes
- PartnerLinQ: What is Electronic Data Interchange (EDI)?
- PartnerLinQ Blog: Integrated vs Stand-Alone EDI Solution
- PartnerLinQ Blog: Why Do Most EDI Practices Struggle to Onboard New Trading Partners
- PartnerLinQ EDI 270 Implementation Guidance.
- Ohio Bureau of Workers’ Compensation EDI 270 v5010 Specification.
- ANSI ASC X12, Transaction Set 270 – Eligibility, Coverage, or Benefit Inquiry.
Explore Our Integration Solutions
PartnerLinQ Integration Solutions
Connect Everything. Integrate Intelligently.
Future-Proof Your Business with Composable, AI Powered Connectivity.



